
Zimbabwe’s public health system is undergoing a dual-track transition, combining post-pandemic infrastructure investment with a forward-looking policy overhaul aimed at aligning service delivery with broader economic ambitions, although questions remain over execution capacity and long-term financing.
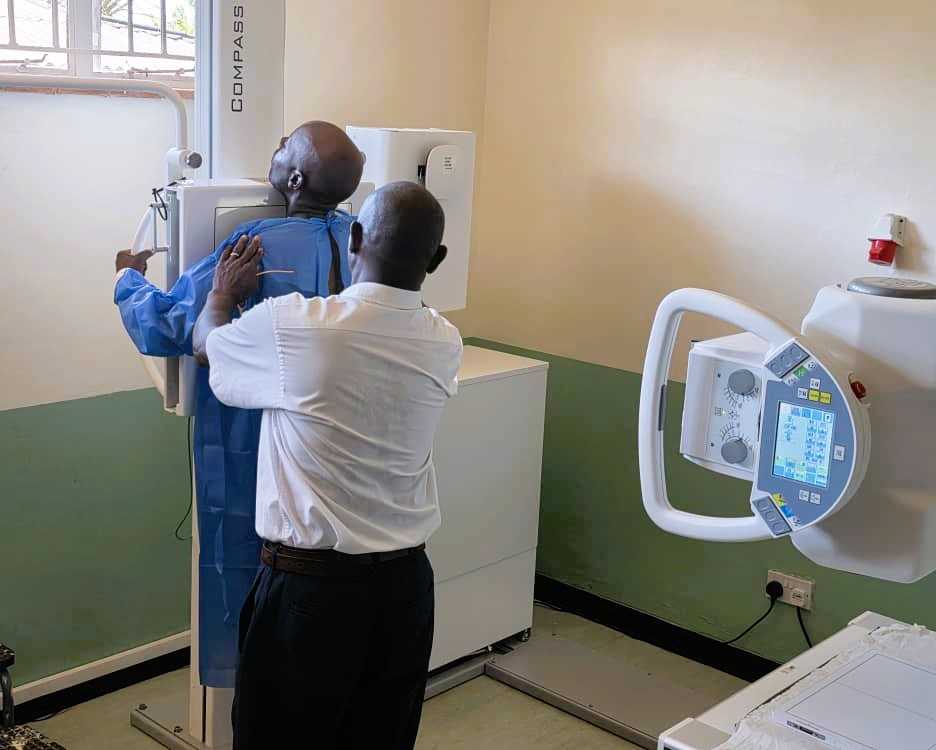
Recent upgrades in Marondera Rural District illustrate how targeted external support is reshaping frontline health delivery. Backed by the Ministry of Health and Child Care in partnership with the Global Fund and United Nations Development Programme Zimbabwe, interventions under the COVID-19 Response Mechanism have focused on strengthening infrastructure resilience and addressing long-standing service delivery gaps.
In practical terms, six health facilities in the district have been equipped with new pharmacies, while 18 facilities have been integrated into Solar for Health programmes. These upgrades are significant in a system where power instability has historically disrupted vaccine cold chains, medicine storage, and basic service provision. Reliable solar energy reduces dependency on an erratic national grid, directly improving operational continuity in rural facilities.
The Ministry said the programme “has strengthened the public health system through the COVID-19 Response Mechanism. This significant investment focuses on improving service delivery and building infrastructure resilience,” adding that in Marondera Rural District, “these efforts have successfully equipped six facilities with new pharmacies and implemented Solar for Health projects at 18 facilities, ensuring consistent power and improved medicine storage.”
These developments reflect a broader shift toward resilience-building in Zimbabwe’s health sector following the COVID-19 pandemic, which exposed structural weaknesses ranging from infrastructure deficits to supply chain vulnerabilities. Investments tied to pandemic recovery have increasingly been repurposed to support long-term system strengthening, particularly in underserved rural areas.
Related Stories
However, while infrastructure gains are measurable, they represent only one layer of a more complex system facing persistent challenges, including staffing shortages, drug availability constraints, and funding gaps. Much of the recent progress remains heavily dependent on donor financing, raising concerns over sustainability once external support tapers.
Parallel to these infrastructure interventions, the government is advancing a policy reset through the development of the National Health Strategy 2026–2030, which is currently undergoing validation at a meeting convened by the Ministry. The strategy is intended to provide a comprehensive roadmap for the sector.
In outlining the process, the Ministry said, “The Ministry of Health and Child Care is hosting a high-level meeting to validate the National Health Strategy 2026-2030. This roadmap ensures every Zimbabwean gets access to quality health care as we move towards becoming an Upper-Middle-Income Economy.” It added that “the NHS2026-30 will ensure that together as a country, we will build a resilient health system that leaves no one and no place behind.”
The policy framework is expected to address alignment between national development goals and health outcomes, resource mobilisation, and governance structures.
Among its stated priorities are ensuring that health strategies are fully costed and realistic, better matching sector priorities with disease burdens, and strengthening accountability mechanisms within the system.
The convergence of infrastructure investment and strategic planning signals an attempt to transition from reactive health responses to a more coordinated and sustainable model. Yet, the gap between policy ambition and implementation remains a defining feature of Zimbabwe’s health sector. Previous strategies have often struggled with underfunding and limited execution capacity, resulting in uneven outcomes across regions.
















Leave Comments