For many women and girls in Zimbabwe, period poverty is often framed as a question of access to sanitary products. For people with disabilities, however, the challenge runs deeper — beyond affordability to systems, infrastructure and policies that were never designed with them in mind.
Inaccessible toilets, unsuitable menstrual products and limited caregiver support continue to turn menstruation into a monthly crisis at the intersection of disability, gender and poverty.
Zimbabwe is home to an estimated more than 1.5 million people living with disabilities, roughly 15 percent of the population, according to disability prevalence estimates used by ZIMSTAT and global health agencies.
Yet menstrual health programmes — including free sanitary wear distribution in schools and communities — largely assume independence, mobility and standard product use. For women and girls with disabilities, this assumption often strips menstruation of dignity, safety and choice.
Disability advocate Shylet says menstruation presents compounded challenges that vary by disability type, exposing the limits of one-size-fits-all interventions.
“Women and girls with disabilities face compounded challenges during menstruation that vary by disability type,” she explains.
For those with physical disabilities, limited mobility and dexterity make changing pads independently and accessing bathrooms difficult, particularly in public spaces where toilets are not wheelchair-friendly. Wheelchair users face additional barriers in cramped stalls that make clothing removal and product changes nearly impossible.
Women and girls with intellectual disabilities often experience confusion around bodily changes, struggle to track menstrual cycles and face heightened vulnerability to exploitation during menstruation.
Visual impairments make it difficult to detect menstrual flow, identify product packaging or dispose of used products hygienically, while sensory sensitivities — particularly among people on the autism spectrum — can turn the texture, smell and unpredictability of menstruation into a source of acute distress.
For those living with chronic pain conditions, menstruation frequently worsens existing pain, with limited access to pain management options that do not interfere with other medication.
Beyond physical barriers, stigma remains pervasive. Shylet notes that many women and girls with disabilities encounter negative attitudes from caregivers, families and institutions that view menstruation as an inconvenience rather than a natural bodily function deserving dignity.
While sanitary products are increasingly available, Shylet argues that current menstrual products largely fail women and girls with disabilities. Standard pads and tampons often require fine motor skills and hand-eye coordination that many people do not have.
Related Stories
Applicators can be difficult to manipulate, while adhesive strips are incompatible with adaptive underwear or incontinence products commonly used by people with disabilities.
Packaging presents another layer of exclusion. Products are often impossible to open independently for those with limited dexterity or vision, and there is no braille labelling or tactile indicators to distinguish absorbency levels. Instructions assume physical capabilities many users do not possess.
For people with disabilities, menstruation also carries a heavier financial burden, as medical costs and reduced employment opportunities limit disposable income, while higher absorbency products or more frequent changes may be required.
In institutional settings, autonomy is further eroded. Shylet points out that people in care facilities are often given whichever product is cheapest or most convenient for staff, rather than what best supports comfort and dignity. Despite growing global conversations on menstrual equity, she notes that the menstrual product market has not innovated for accessibility, leaving major design gaps unaddressed.
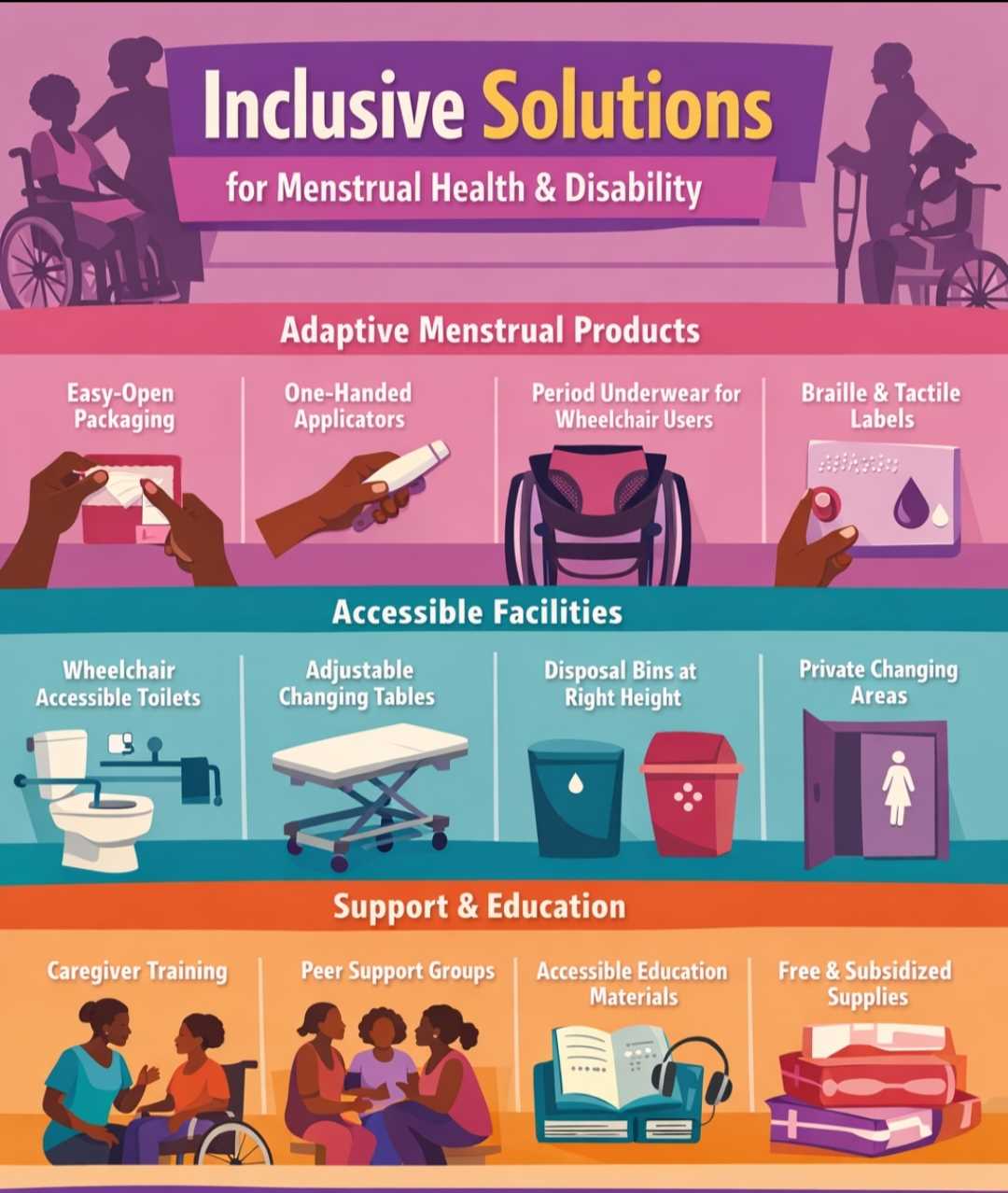
Yet solutions are emerging — and they point to inclusive design rather than charity-based responses. Shylet outlines a range of product innovations that could transform menstrual experiences for people with disabilities, including easy-grip, one-handed applicators, magnetic or snap closures instead of adhesive, extended-wear products for those unable to change frequently, braille and tactile labelling, sensory-friendly materials and products compatible with adaptive clothing and mobility devices.
Period underwear designed specifically for wheelchair users, she says, would address a long-standing gap.
Infrastructure remains a critical part of the solution. Disability-friendly water, sanitation and hygiene (WASH) facilities are still rare in Zimbabwean schools, clinics and public spaces, despite the country’s commitments under the Constitution and the National Disability Policy. Accessible bathrooms with adequate space, support bars, adjustable-height changing tables, private changing areas and disposal units positioned at appropriate heights are essential for dignified menstrual management. Without them, even free sanitary products remain functionally inaccessible.
Support systems also matter. Shylet stresses the need for dignity-centred caregiver training, peer support networks for women with disabilities, personal care attendants trained specifically in menstrual support, subsidised products and menstrual tracking tools with accessibility features. These interventions, she argues, empower rather than control, and centre independence wherever possible.
Despite their lived expertise, women and girls with disabilities remain largely excluded from menstrual health conversations. Shylet notes that most menstrual health programmes focus on “typical” users, with disability addressed, if at all, as an afterthought. Research rarely disaggregates menstrual health data by disability status, rendering specific challenges invisible in policy-making. In schools, menstrual education assumes all students can independently manage their periods, while special education settings may avoid the topic entirely.
This exclusion, she says, violates the principle of “Nothing About Us Without Us”, perpetuating a cycle where needs remain unmet and dignity compromised. The gaps are evident across information, products, infrastructure, services and policy. Menstrual education materials are rarely available in braille, audio, sign language or easy-read formats. Public bathrooms remain inaccessible, particularly in rural areas. Health workers receive little training on disability-inclusive menstrual health, and national menstrual equity efforts do not explicitly integrate disability into budgeting or standards.
Still, Shylet points to inclusive solutions that are already working, albeit on a limited scale. Peer-led initiatives by organisations of women with disabilities are creating adaptive strategies and community support networks. Small innovators are developing magnetic-closure pads and wheelchair-friendly period underwear, while some disability organisations have produced accessible menstrual education materials with measurable improvements in confidence and knowledge. These initiatives succeed, she says, because they are co-designed with disabled women, grounded in lived experience rather than assumptions.
Ending period poverty for people with disabilities in Zimbabwe will require a shift from temporary fixes to systemic change. It demands products designed for diverse bodies, infrastructure built for inclusion and policies that recognise menstrual health as a human rights issue. Most importantly, it requires listening to women with disabilities — not as beneficiaries, but as experts.

















Leave Comments